The number of suspected overdose/poisoning paramedic calls in Mission has almost doubled in 2017 compared to the same time period in 2016.
According to statistics provided by BC Emergency Health Services, in a seven-month period (from April to October 2016) there were approximately 61 paramedic calls in Mission for suspected overdose/poisoning. In the same period in 2017, the number of Mission calls shot up to 111.
How many of those 111 calls involved an overdose fatality cannot be publicly determined.
According to the BC Coroner’s Office, Mission has fewer than five overdose fatalities per month. More specific numbers are not available.
“We don’t release that data due to both privacy concerns and potential fluctuation/variability in data we compile,” explained Andy Watson, manager of strategic communications for the BC Coroners Service.
He wrote in an email to The Record that post-mortem testing can reveal different details in suspected cases, and cases previously not suspected to be related to illicit drugs can impact small numbers, so the coroner’s service does not share anything under five fatalities a month.
Mission’s increase in overdose calls is not out of the ordinary as the province has also been experiencing a surge in calls.
In April 2016 there was a declaration of a public health overdose emergency. At that time, Fraser Health implemented a “multi-faceted response strategy” in the region.
“This strategy is founded on the pillars of prevention, harm reduction and treatment and has evolved throughout the public health emergency,” explained Tasleem Juma, senior consultant of public affairs for Fraser Health.
“The strategy focuses on identifying and implementing priority sites for supervised consumption and overdose prevention services, increasing accessibility and administration of naloxone and Take Home Naloxone, launching public awareness campaigns, engaging with municipal and community partners on overdose response and prevention, and improving access to opioid agonist treatment,” Juma wrote in an email.
“Through the Mission Active Support Table we collaborate with Mission service providers to identify at-risk individuals and provide support to them before they are in a state of crisis.”
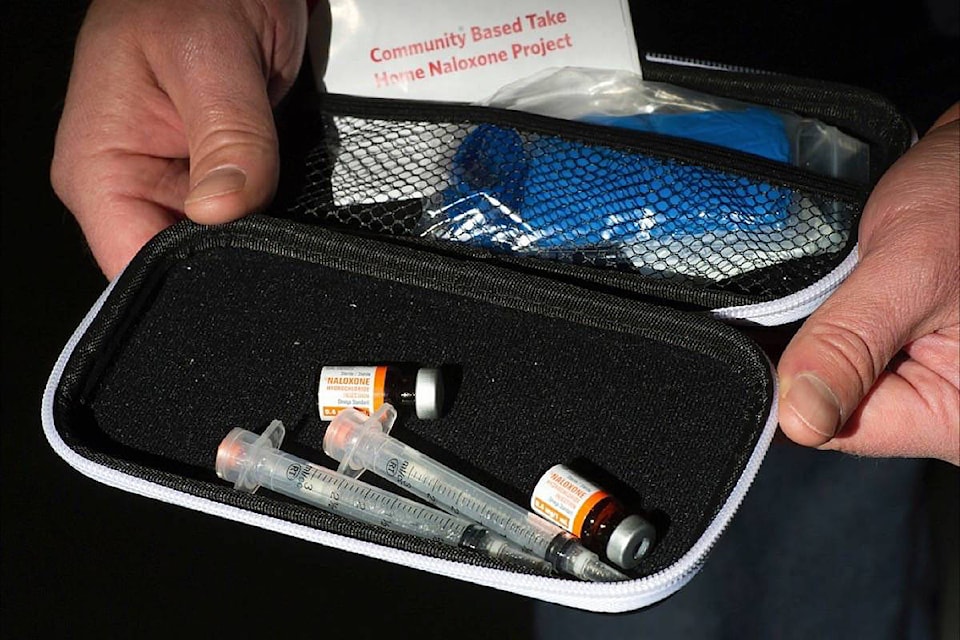
In Mission, naloxone training is available through the Mission Public Health Unit, Mission Friendship Centre Society and Positive Living Fraser Valley’s mobile health van.
A number of community organizations have already been trained in the use of Take Home Naloxone, including Mission Youth (MY) House, Mission Friendship Centre, Mission Ministry of Children and Family Development, and Fraser House Society.
Take Home Naloxone kits and harm-reduction supplies are also available at Mission Public Health Unit, Mission Friendship Centre Society, and Positive Living Fraser Valley’s mobile health van.
“In addition to better access to naloxone, we have increased access to opioid agonist treatment, an evidence-based treatment that uses medications such as Suboxone or methadone to stabilize a person who is addicted to substances and reduces harms associated with opioid use,” Juma said.
Fraser Health is planning to open an opioid agonist treatment clinic in Mission early in the new year.
Juma said there are many reasons why people use alcohol, tobacco and other drugs.
“Our job as health care providers and community members is to understand that those reasons can be very complex, potentially connected to trauma, mental health and emotional or physical pain, and look to find ways to reduce harm and facilitate connections to support.”
She said the stigma toward people struggling with mental health and substance use issues keeps people from asking for help and further marginalizes them. It also creates barriers for people to access health and social services, including treatment.